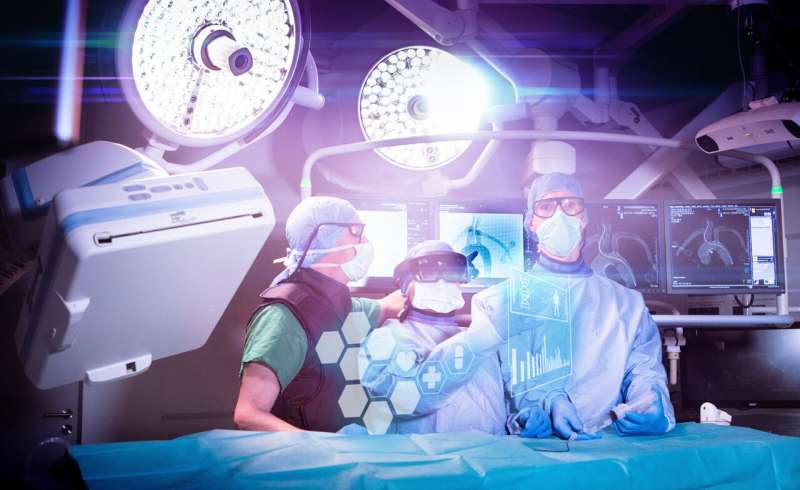
In the future, artificial intelligence will assist neuroradiologists during endovascular surgery. Credit: Fraunhofer-Gesellschaft
When a patient has a stroke, every minute counts. Here, prompt action can prevent serious brain damage. If a clot is blocking a large blood vessel in the brain, surgeons can remove this occlusion by means of a catheter inserted in the patient's groin. However, this is a complicated procedure, requiring a lot of experience, and only a few specialists are capable of carrying it out. In new work, Fraunhofer researchers have been investigating whether artificial intelligence might be used to steer a catheter automatically and reliably to a blocked blood vessel. Initial tests with a simulation model and in the laboratory have been highly promising. The research team will be demonstrating this new technique on a blood vessel phantom at the MEDICA 2019 trade fair in Düsseldorf from November 18 to 21 (Hall 10, Booth G05).
In Germany, around 270,000 people suffer from a stroke each year. This sudden disruption to the supply of blood in the brain requires prompt medical attention. If not treated in time, a significant number of brain cells can die, leaving the patient with lasting damage such as paralysis or a speech impediment. In the worst case, it can prove fatal. Increasingly, the therapy of choice is a so-called thrombectomy. Here, a thin catheter is inserted into an artery, via the groin, and advanced to the aorta, from where it is threaded all the way up to the blocked blood vessel in the brain. Once the blocked vessel has been reached, a special instrument known as a stent retriever is opened to reveal a tiny, basket-like mesh that becomes firmly entangled with the blood clot. The catheter is then withdrawn, along with the clot. This procedure takes anything from 45 minutes to three and a half hours, depending on the skill of the operator. The ability to conduct a thrombectomy requires long training and plenty of practice. Depending on the specific case, anything between ten minutes and one and a half hours are required to navigate the catheter to the blood clot. Researchers from the Mannheim-based Project Group for Automation in Medicine and Biotechnology PAMB—which is affiliated to the Fraunhofer Institute for Manufacturing Engineering and Automation IPA—have been taking a closer look at this problem. Their idea is to use a robotic system—in the form of a computer-controlled catheter—to establish a faster and more reliable alternative to this painstaking procedure. In a new departure, they have harnessed the power of artificial intelligence to guide the catheter autonomously to the site of interest. "The surgical intervention itself, in which the blood clot is removed by means of the stent retriever, is still carried out by a physician. But the actual journey to the blocked blood vessel, where various anatomical difficulties have to be negotiated, is undertaken solely by an autonomously controlled catheter," explains Johannes Horsch, one of the project group's engineering scientists. "This procedure can be used not only for removing blood clots but also in other types of endovascular surgery, such as treatment for cardiac infarction or liver tumors."
Autonomous navigation based on deep reinforcement learning
The species of artificial intelligence that enables the catheter to navigate autonomously is known as deep reinforcement learning (DRL). This is one of the methods used to train neural networks, and it closely resembles the way in which people learn. The specific characteristic of DRL is that the data used to train the neural network are automatically generated by an algorithm in the course of repeated practice on a computer simulation model—in this instance, a virtual reconstruction of the vascular tree and a catheter, with which the algorithm interacts. In addition, the researchers have developed a second algorithm to evaluate whether the action taken is right or wrong. If, for example, the guidewire is correctly turned to the right and inserted into the correct blood vessel at the next junction, the first algorithm is awarded one or more plus points, e.g., +1. If, however, the algorithm makes an incorrect decision, a minus point is awarded. This feedback enables the algorithm to learn autonomously, so that the neural network continuously adapts and improves. "Using the model, we can simulate all the possible movements of the catheter and train the neural network to a certain level," Horsch says. "So far, we've had a 95 percent success rate with the simulation model—i.e., in a simplified scenario, the catheter was autonomously navigated to the blocked blood vessel without problem. Our aim is to nudge that up to 99 percent by the start of MEDICA."
For autonomous navigation to function in an actual surgical intervention, the position of the catheter must be tracked in real time. This is where another project partner, the Fraunhofer Institute for Digital Medicine MEVIS, enters the picture. Researchers there are developing an intelligent catheter, which is tracked in the vascular system via fiber-optic sensors and without any imaging. In addition, they are using fluoroscopic images to train a neural network to withdraw the catheter through the vascular system. The next step will be to take these results, generated with a simulation model, and transfer them to a phantom—i.e., a model, made of plastic, of the entire blood vessel tree from the groin to the brain.
Packed with the practical knowledge of many experienced surgeons
A lot of experience from practicing physicians has flowed into building an algorithm that will navigate the catheter swiftly and reliably through the vascular system. A key benefit of this new technology is that it will narrow the huge variation in the time taken for such a procedure—a variation that is the result of differences in patient anatomy. Equally important, it will enable smaller clinics, without trained specialists in this field, to offer endovascular stroke therapy. At present, only specialized stroke units have the relevant equipment and medical expertise to carry out such treatment.
Catheter threaded over and along the guidewire
For the moment, the researchers are using a guidewire in the simulation tests. The next step will be to try navigating a catheter which is threaded over and along the guidewire like a sheath. "In current practice, the catheter follows the guidewire. Once the guidewire has reached the right blood vessel, the catheter is pushed into place," Horsch explains. The team is hoping to develop the use of two or three increasingly fine catheters, one inserted inside the other, so that the smallest will fit inside the minuscule blood vessels in the brain, which are much narrower than the blood vessels in the groin region.
The project is scheduled to run until September 2020. By then, the researchers will have completed preclinical testing on the silicon phantom of the blood vessel tree and perfected the algorithm used to navigate the catheter. Follow-up projects will then focus on optimizing the procedure, in particular with regard to its safety and reliability. After that, a further four to five years have been set aside for clinical studies to demonstrate its safety and efficacy. "It will no doubt take another ten to 15 years before the system can be commercialized for use in hospitals," Horsch says. "Before then, a lot of research work and clinical studies will be required. And, in addition to all that, lawmakers will have to issue regulatory approval for the use of neural networks in a medical context." Horsch and his colleagues will be demonstrating the latest results of their research at the MEDICA trade fair in Düsseldorf from November 18 to 21, 2019 (Hall 10, Booth G05).
Provided by Fraunhofer-Gesellschaft