June 26, 2015 weblog
Tissue-penetrating approach involves MRI-powered millirobots
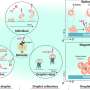
Last month at the 2015 IEEE International Conference on Robotics and Automation (ICRA) in Seattle a team presented their work, "Toward Tissue Penetration by MRI-powered Millirobots Using a Self-Assembled Gauss Gun.". Their work suggests an approach for the MRI-based navigation and propulsion of millirobots for minimally invasive therapies. They discussed a technique for generating large impulsive forces to penetrate tissue. Aaron T. Becker, Ouajdi Felfoul and Pierre E. Dupont authored the study.
Millimeter-scale robots have the potential to provide highly localized therapies with minimal trauma by navigating through the natural fluid-filled passageways of the body.
In certain cases, however, there is a challenge when forces required for tissue penetration are substantially higher than those needed to propel a millirobot through a bodily fluid. This can be difficult. They suggested, though, there is a way. As IEEE Spectrum's headline on Thursday put it, "Self-assembling robotic gun will shoot through tissue inside your body."
The approach, according to the paper, "involves navigating individual millirobots to a target location and allowing them to self-assemble in a manner that focuses stored magnetic potential energy as kinetic energy for tissue penetration." The concept, said the authors, corresponds to a Gauss gun or accelerator.
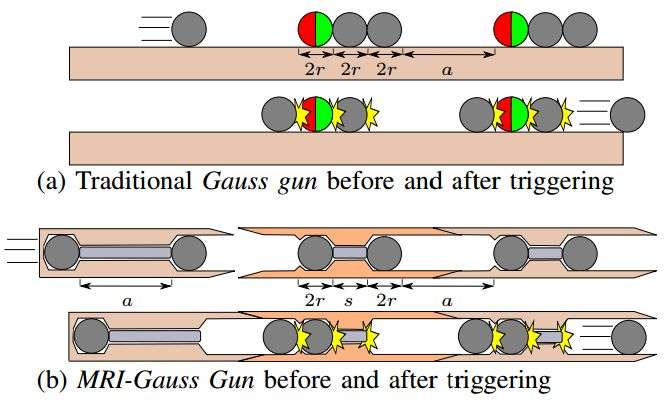
"The traditional Gauss gun depends on permanent magnets and steel spheres. To use stored magnetic potential energy, a new MRI Gauss gun was designed. The MRI Gauss gun can be self-assembled into a larger tool to increase puncture force, far stronger than the forces possible with MRI gradients," they wrote.
What is a Gauss gun? Evan Ackerman in IEEE Spectrum described it as a "kind of a magnetic accelerator, but it works a bit differently. It uses the principle of conservation of momentum to transfer force through a series of magnets, turning stored magnetic potential energy into kinetic energy."
He added, "In principle, the self-assembling Gauss gun works the same way, using little magnetic robots steered by an MRI machine."
Fundamentally, they have shown, said Ackerman, "how a small swarm of robots can turn themselves into a Gauss gun, firing projectiles that can penetrate tissue."
The authors are from University of Houston (Aaron Becker is assistant professor in the Electrical and Computer Engineering department) and Boston Children's Hospital.
Their experiments were performed using a clinical MRI scanner. "Future work," the authors said, "should investigate how the design can be optimized for clinical use cases and implement closed-loop control of the components."
Felfoul, one of the co-authors, is working on robotic projects that use MRI systems to power, control and image tetherless surgical robots, under a surgeon's guidance and control.
In May, a news story by Elena Watts on the University of Houston news site, reported on Becker's work with the Boston team; in her report, Becker discussed the authors' research in the context of a real-world surgical example.
Hydrocephalus, she noted, is where "accumulating fluid in the skull ratchets up pressure on the brain and can cause lifelong mental disabilities. Current treatment requires physicians to cut through the skull and implant pressure-relieving shunts."
"Hydrocephalus, among other conditions, is a candidate for correction by our millirobots because the ventricles are fluid-filled and connect to the spinal canal," Becker said. "Our noninvasive approach would eventually require simply a hypodermic needle or lumbar puncture to introduce the components into the spinal canal, and the components could be steered out of the body afterwards."
More information: Toward Tissue Penetration by MRI-powered Millirobots Using a Self-Assembled Gauss Gun, 2015 IEEE International Conference on Robotics and Automation (ICRA), (PDF)
© 2015 Tech Xplore