Improved brain chip for precision medicine

The Akay Lab biomedical research team at the University of Houston is reporting an improvement on a microfluidic brain cancer chip previously developed in their lab. The new chip allows multiple-simultaneous drug administration, and a massive parallel testing of drug response for patients with glioblastoma (GBM), the most common malignant brain tumor, accounting for 50% of all cases. GBM patients have a five-year survival rate of only 5.6%.
"The new chip generates tumor spheroids, or clusters, and provides large-scale assessments on the response of these GBM tumor cells to various concentrations and combinations of drugs. This platform could optimize the use of rare tumor samples derived from GBM patients to provide valuable insight on the tumor growth and responses to drug therapies," reports Metin Akay, John S. Dunn Endowed Chair Professor of Biomedical Engineering and department chair. The paper is published in the inaugural issue of the IEEE Engineering in Medicine & Biology Society's Open Journal of Engineering in Medicine and Biology.
The ability to quickly assess the effectiveness of a cancer drug would be a notable improvement over typical cancer protocols in which chemotherapy drugs are given, then tested for several months, and a patient switched to another drug if the first is ineffective. The new device can determine the optimal drug combination in as little as two weeks. "When we can tell the doctor that the patient needs a combination of drugs and the exact proportion of each, this is precision medicine."
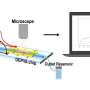
Akay's team takes a piece of a tumor biopsy, cultures it and puts it in the chip. Then they add chemotherapy drugs to the chip's microvalves to determine the best drug combination, and the specific proportion, that kills the most tumor cells.
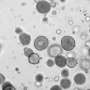
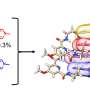
The team cultured 3-D tumor spheroids, or clusters, from GBM cell lines as well as patient-derived GBM cells in vitro and investigated the effect of the combination of Temozolomide and a nuclear factor-κB inhibitor on tumor growth.
"Our study revealed that these drugs have synergistic effects in inhibiting spheroid formation when used in combination, and suggests that this brain cancer chip enables large-scale, inexpensive and sample-effective drug screening to 3-D cancer tumors in vitro. Further, this platform could be applied to related tissue engineering drug screening studies," said assistant professor Yasmine Akay. She is joined on the team by research assistant professor Naze Gul Avci and post-doctoral fellow Hui Xia. The tissue samples were provided by project collaborator Jay-Jiguang Zhu, MD, director, Neuro Oncology, McGovern Medical School at UT Health.
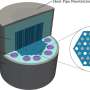
To minimize any sample loss in vitro, the team improved their existing brain cancer chip system by adding an additional laminar flow distribution layer, which reduces sample loss during cell seeding and prevents spheroids from escaping. This allows the spheroids to form uniformly throughout the chip for consistent drug testing between each spheroid.
More information: Hui Xia et al, Temozolomide in Combination with NF-κB Inhibitor Significantly Disrupts the Glioblastoma Multiforme Spheroid Formation, IEEE Open Journal of Engineering in Medicine and Biology (2019). DOI: 10.1109/OJEMB.2019.2962801