November 28, 2017 report
A way to monitor vital signs without touching patients
(Tech Xplore)—A pair of researchers at Cornell University has developed a new way to monitor vital signs in patients—one that does not require direct contact with the skin. In their paper published in the journal Nature Electronics, Xiaonan Hui and Edwin Kan describe the nature of the device and how it can be used.
Anyone who has spent time in a hospital knows that the means used to measure vital signs is restrictive, and in some cases (such as when the tape securing them is pulled), can even be painful. In this new effort, the researchers have come up with a way to offer healthcare providers the same information on patients without having to touch them.
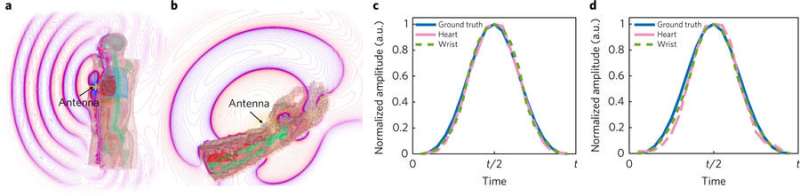
The new device is based on RFID chip technology—the same technology used in key fobs. It works by sending a radio signal into the body and then listening to the signal that comes back (rather like sonar) and relaying what it finds to a nearby processing unit. Hui and Kan discovered that the simple technology could be used to monitor vital signs if programed in specific ways. By sending a signal into the chest, for example, and noting slight disturbances in the signal that is sent back, the device is able to monitor breathing activity. In roughly the same way, it can also monitor the heartbeat. And by placing another of the devices near the wrist, it can be used to measure blood pressure by calculating elapsed time between heartbeats.
Because the device is so small, the researchers note, it could be sewn into a hospital gown or a bed sheet. In such an arrangement, each patient would be monitored by one or more of the devices without attaching anything to the body. They point out that the technology could actually be used to monitor more than one patient if need be. And they further note that because the hardware already exists, using it to monitor patients would be inexpensive and easy to use by hospital staff. They claim the devices are hardy, as well—they sent some through a clothes-washing machine a few times, and report that it still worked perfectly.
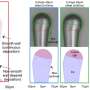
![The RFID tag prototypes. (a) An RFID sensor tag chip integrated with the embroidered antenna on fabric. (b) The PCB prototype of the harmonic RFID tag for NCS. Credit: Nature Methods (2017). DOI: 10.1038/nmeth.4498 Researchers demonstrate that lung stem cells can help regenerate injured lungs in laboratory mice [rejected]](https://scx1.b-cdn.net/csz/news/800a/2017/5a1d4fd3e104a.jpg)
More information: Xiaonan Hui et al. Monitoring vital signs over multiplexed radio by near-field coherent sensing, Nature Electronics (2017). DOI: 10.1038/s41928-017-0001-0
Abstract
Monitoring the heart rate, blood pressure, respiration rate and breath effort of a patient is critical to managing their care, but current approaches are limited in terms of sensing capabilities and sampling rates. The measurement process can also be uncomfortable due to the need for direct skin contact, which can disrupt the circadian rhythm and restrict the motion of the patient. Here we show that the external and internal mechanical motion of a person can be directly modulated onto multiplexed radiofrequency signals integrated with unique digital identification using near-field coherent sensing. The approach, which does not require direct skin contact, offers two possible implementations: passive and active radiofrequency identification tags. To minimize deployment and maintenance cost, passive tags can be integrated into garments at the chest and wrist areas, where the two multiplexed far-field backscattering waveforms are collected at the reader to retrieve the heart rate, blood pressure, respiration rate and breath effort. To maximize reading range and immunity to multipath interference caused by indoor occupant motion, active tags could be placed in the front pocket and in the wrist cuff to measure the antenna reflection due to near-field coherent sensing and then the vital signals sampled and transmitted entirely in digital format. Our system is capable of monitoring multiple people simultaneously and could lead to the cost-effective automation of vital sign monitoring in care facilities.
© 2017 Tech Xplore